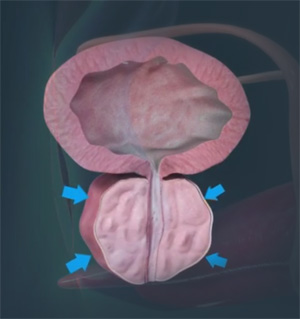
What is Enlarged Prostate or Benign Prostatic Hypertrophy?
Benign prostatic hypertrophy or BPH is a non-cancerous enlargement of the prostate gland. It is also referred to as benign prostatic hyperplasia. It is not uncommon for the prostate gland to become enlarged as men age. When the prostate gland becomes enlarged, it can cause problems with urination.
It is common for the prostate gland to become enlarged as a man ages. Doctors call this condition benign prostatic hyperplasia (BPH), or benign prostatic hypertrophy. As the prostate enlarges, the layer of tissue surrounding it stops it from expanding, causing the gland to press against the urethra like a clamp on a garden hose. The bladder wall becomes thicker and irritable. The bladder begins to contract even when it contains small amounts of urine, causing more frequent urination. Eventually, the bladder weakens and loses the ability to empty itself, so some of the urine remains in the bladder. The narrowing of the urethra and partial emptying of the bladder cause many of the problems associated with BPH.
Symptoms of Enlarged Prostate
BPH rarely causes symptoms before age 40, but more than half of men in their sixties and as many as 90 per cents in their seventies and eighties have some symptoms of BPH. Many symptoms of BPH stem from obstruction of the urethra and gradual loss of bladder function, which results in incomplete emptying of the bladder. The symptoms of BPH vary, but the most common ones involve changes or problems with urination, such as: hesitant, interrupted, weak stream urgency and leaking or dribbling more frequent urination, especially at night.
Sometimes, a man may not know he has any obstruction until he suddenly finds himself unable to urinate at all. This condition, called acute urinary retention, may be triggered by taking over-the-counter cold or allergy medicines. Such medicines contain a decongestant drug, known as a sympathomimetic. A potential side effect of this drug may prevent the bladder from opening from relaxing and allowing urine to empty. When partial obstruction is present, urinary retention also can be brought on by alcohol, cold temperatures, or a long period of immobility.
Causes of Enlarged Prostate
The cause of BPH is not well understood. No definite information on risk factors exists. For centuries, it has been known that BPH occurs mainly in older men and that it doesn't develop in men whose testes were removed before puberty. For this reason, some researchers believe that factors related to ageing and the testes may spur the development of BPH.
One theory focuses on DHT, a substance made from testosterone in the prostate that may help control prostate growth. The accumulation of DHT in older men may encourage the growth of cells leading to BPH.
Another theory suggests elevated estrogen levels that occur as men age may increase cellular growth activity leading to BPH.
Diagnosis of Enlarged Prostate
You may first notice symptoms of BPH yourself, or your doctor may find that your prostate is enlarged during a routine checkup. When BPH is suspected, you may be referred to a urologist, a doctor who specializes in problems of the urinary tract and the male reproductive system. Some tests your doctor may order can include the following:
- Digital Rectal Examination (DRE): This examination is usually the first test done. The doctor inserts a gloved finger into the rectum and feels the part of the prostate next to the rectum. This examination gives the doctor a general idea of the size and condition of the gland.
- Prostate-Specific Antigen (PSA) Blood Test: To rule out cancer as a cause of urinary symptoms, your doctor may recommend a PSA blood test. PSA, a protein produced by prostate cells, is frequently present at elevated levels in the blood of men who have prostate cancer. The U.S. Food and Drug Administration (FDA) has approved a PSA test for use in conjunction with a digital rectal examination to help detect prostate cancer in men who are age 50 or older and for monitoring men with prostate cancer after treatment. However, much remains unknown about the interpretation of PSA levels, the test's ability to discriminate cancer from benign prostate conditions, and the best course of action following a finding of elevated PSA.
- Rectal Ultrasound and Prostate Biopsy: If there is a suspicion of prostate cancer, your doctor may recommend a test with rectal ultrasound. In this procedure, a probe inserted in the rectum directs sound waves at the prostate. The echo patterns of the sound waves form an image of the prostate gland on a display screen. To determine whether an abnormal-looking area is indeed a tumour, the doctor can use the probe and the ultrasound images to guide a biopsy needle to the suspected tumour. The needle collects a few pieces of prostate tissue for examination with a microscope.
- Urine Flow Study: Your doctor may ask you to urinate into a special device that measures how quickly the urine is flowing. A reduced flow often suggests BPH.
- Cystoscopy: In this examination, the doctor inserts a small tube through the opening of the urethra in the penis. This procedure is done after a solution numbs the inside of the penis so all sensation is lost. The tube, called a cystoscope, contains a lens and a light system that help the doctor see the inside of the urethra and the bladder. This test allows the doctor to determine the size of the gland and identify the location and degree of the obstruction.
Treatment for Enlarged Prostate
Conservative treatment measures to treat BPH are always considered first before invasive measures such as surgery. Some conservative treatment measures include the following:
Medications: Medications are the most common treatment method for controlling symptoms of BPH. There are a number of medications approved for the treatment of BPH symptoms. Some prevent the growth of the prostate while others actually shrink the prostate gland. Other drugs may be prescribed to improve urine flow and reduce bladder outlet obstruction. Your doctor will discuss the various drugs available to treat your particular condition.
Non-surgical treatment measures are minimally invasive treatments to reduce the size of the prostate gland and enlarge the urethra to make voiding easier. These may include the following:
- Transurethral Microwave Therapy (TUMT): Cooled Thermotherapy is a non-surgical, office-based prostate therapy used to treat BPH in a 30-minute treatment. Cooled Thermotherapy uses precisely targeted microwave energy to heat and destroy enlarged prostate tissue while a cooling mechanism protects healthy, surrounding tissue. This non-surgical BPH treatment is performed on an outpatient basis and requires local anaesthesia and/or oral medications. Within weeks, the majority of men notice the improvement in their symptoms and overall quality of life.
-
Transurethral Needle ablation (TUNA): The TUNA system delivers low-level radiofrequency energy through twin needles to burn away a well-defined region of the enlarged prostate.
Shields protect the urethra from heat damage. The TUNA system improves urine flow and relieves symptoms with fewer side effects when compared with transurethral resection of the prostate (TURP) surgery. No incontinence or impotence has been observed. - Water-induced thermotherapy: This therapy uses heated water to destroy excess tissue in the prostate. A catheter containing multiple shafts is positioned in the urethra so that a treatment balloon rests in the middle of the prostate. A computer controls the temperature of the water, which flows into the balloon and heats the surrounding prostate tissue. The system focuses the heat in a precise region of the prostate. Surrounding tissues in the urethra and bladder are protected. Destroyed tissue either escapes with urine through the urethra or is reabsorbed by the body.
- Laser treatment for BPH: is also called laser prostatectomy. The permanent effects of laser treatment on prostate tissue are vaporization and coagulation, which occur when laser energy heats prostatic tissue to 100°C. At this temperature, tissue death occurs, resulting in shrinkage of the prostate over time. This process can initially cause oedema, which may increase prostate volume and make short-term catheterization necessary for voiding.




